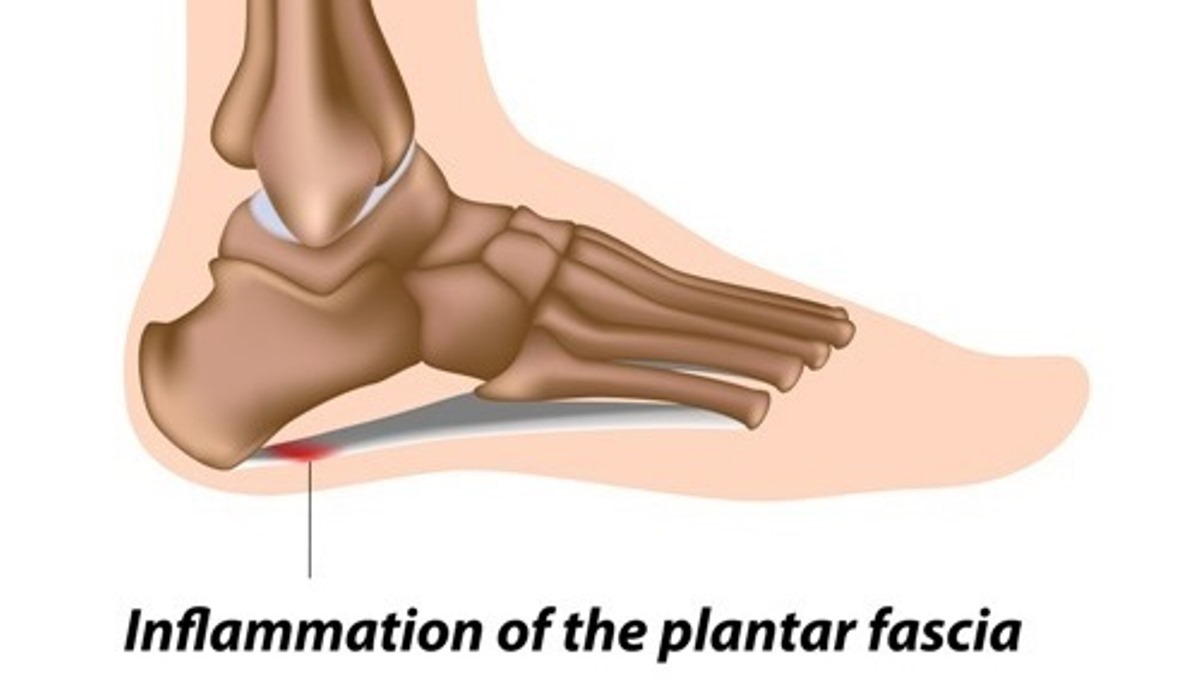
The plantar fascia is the thick tissue on the bottom of the foot. It connects the heel bone to the toes and creates the arch of the foot. When this tissue becomes swollen or inflamed, it is called plantar fasciitis.
Causes
Swelling occurs when the thick band of tissue on the bottom of the foot (fascia) is overstretched or overused. This can be painful and make walking more difficult.
You are more likely to get plantar fasciitis if you:
- Have foot arch problems (both flat feet and high arches)
- Run long distances, downhill or on uneven surfaces
- Are obese or gain weight suddenly
- Have a tight Achilles tendon (the tendon connecting the calf muscles to the heel)
- Wear shoes with poor arch support or soft soles
- Change your activities
Plantar fasciitis is seen in both men and women. It is one of the most common orthopedic foot complaints.
Plantar fasciitis was commonly thought to be caused by a heel spur. However, research has found that this is not the case. On x-ray, heel spurs are seen in people with and without plantar fasciitis.
Symptoms
The most common symptom is pain and stiffness in the bottom of the heel. The heel pain may be dull or sharp. The bottom of the foot may also ache or burn.
The pain is often worse:
- In the morning when you take your first steps
- After standing or sitting for awhile
- When climbing stairs
- After intense activity
- Walking, running, and jumping sports
The pain may develop slowly over time, or come on suddenly after intense activity.
Exams and Tests
The health care provider will perform a physical exam. This may show:
- Pain on the bottom of your foot.
- Pain along the sole of the foot.
- Flat feet or high arches.
- Mild foot swelling or redness.
- Stiffness or tightness of the arch in the bottom of your foot.
X-rays may be taken to rule out other problems.
Treatment
Your provider will often recommend these steps first:
- Heel and foot stretching exercises
- Resting as much as possible for at least a week
- Wearing shoes with good support and cushions
If these treatments do not work, your provider may recommend:
- Wearing a boot cast, which looks like a ski boot, for 3 to 6 weeks. It can be removed for bathing.
- Custom-made shoe inserts (orthotics)
- Steroid shots or injections into the heel
Sometimes, foot surgery is needed.
Outlook (Prognosis)
Nonsurgical treatments almost always improve the pain. Treatment lengths can vary on each individual patient.
When to Contact a Medical Professional
Contact your provider if you have symptoms of plantar fasciitis.
Prevention
Making sure your ankle, Achilles tendon, and calf muscles are flexible can help prevent plantar fasciitis. Stretch your plantar fascia in the morning before you get out of bed. Doing activities in moderation can also help.